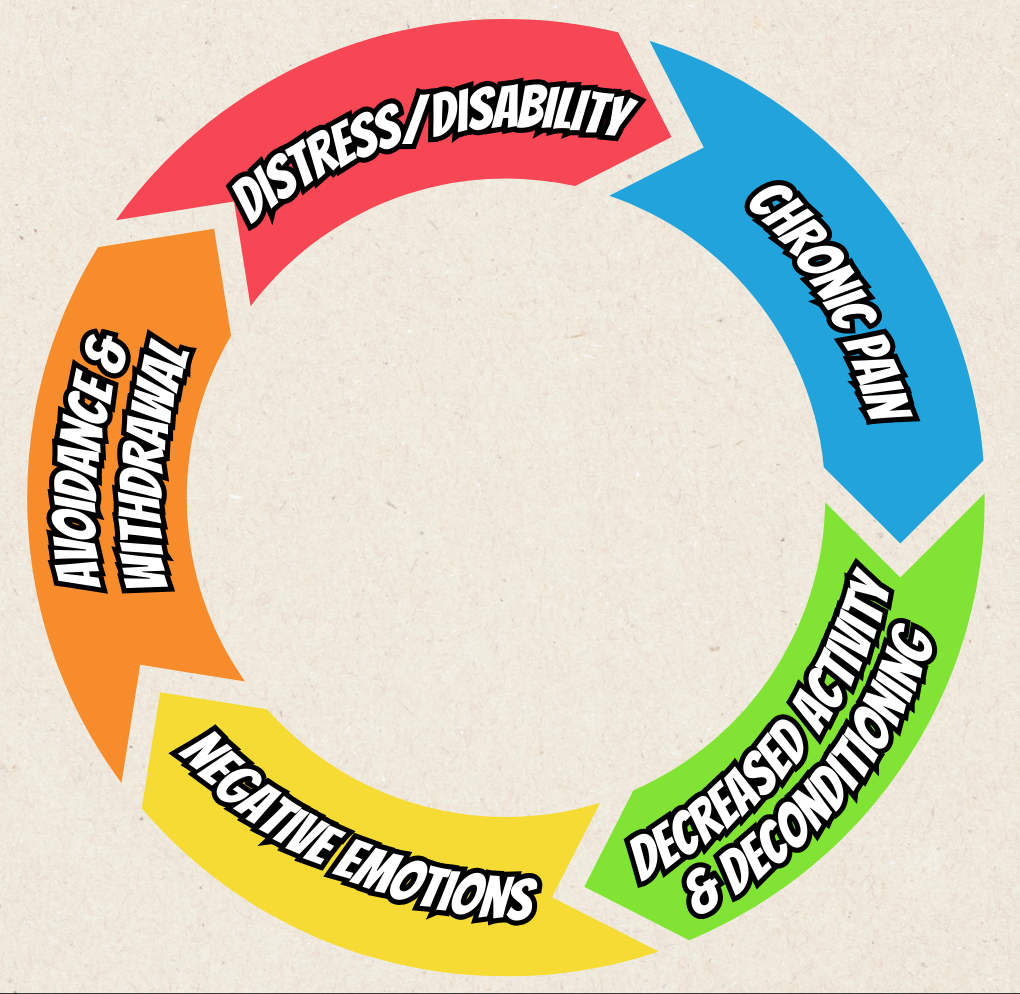
Chronic Pain Cycle
“Healing takes courage, and we all have courage, even if we have to dig a little to find it.” — Tori Amos
Chronic pain isn’t “just in your head” – it’s a complex experience that affects your body, mind, and life in a self-perpetuating loop. When we hurt constantly, it’s natural to become less active and more withdrawn, which can unfortunately increase pain over time. This chronic pain cycle can trap us in a feedback loop of pain → inactivity → low mood → even more pain. The good news is that by understanding this cycle, we can find compassionate ways to break it and reclaim a sense of control and hope.
In many cultures and pain management approaches, chronic pain is seen through a biopsychosocial lens – meaning biological, psychological, and social factors all play a role. For example, an injury or health condition may start the pain, but then our muscles weaken from lack of activity, our mood and thoughts turn negative (“I can’t do anything anymore”), and we avoid activities or people we love. This avoidance can lead to loneliness, disability, and even more sensitivity to pain. Clinicians have termed this the Chronic Pain Cycle – a vicious circle where pain feeds into suffering and vice versa. Understanding this cycle isn’t about blaming yourself; it’s about empowering you with knowledge. It shows that pain is not your fault – it’s a whole-body experience – and that there are points where you can intervene to ease the spiral.
Steps to Break the Pain Cycle
Taking small, gentle steps can gradually interrupt the pain cycle. Here are some practical strategies:
- Pace and Move Gently: Try gradual, safe activity to prevent deconditioning. Even a short walk or gentle stretch, done regularly, can keep your body from getting weaker. Remember the saying “motion is lotion” – a little movement (within your limits) can lubricate joints, build strength, and release endorphins to reduce pain.
- Relaxation and Breathing: Practice relaxation techniques to calm your nervous system. Deep breathing, warm baths, or progressive muscle relaxation (tensing and releasing muscles) can reduce tension that heightens pain signals. When pain flares, pause, inhale slowly, and tell yourself “It’s okay; let me soften around the pain” as you exhale.
- Challenge Negative Thoughts: Notice catastrophic thoughts like “I’ll always feel this bad.” Gently question these thoughts – are they 100% true? Often, pain has good days and bad days. Remind yourself of what is still possible (“Today is hard, but other days have been better”). Reframing hopeless thoughts can lift your mood and lower perceived pain.
- Stay Socially Connected: Pain can make us want to isolate, but supportive contact (even a phone call or brief visit) can lift your spirits. Let trusted friends or family know when you’re struggling. Even if you can’t do physical activities together, having someone listen or simply sit with you can ease the emotional burden of pain.
- Work with Professionals: Don’t hesitate to use medical and therapeutic support. Pain specialists, physical therapists, or counselors (especially those trained in pain-focused CBT or ACT) can offer tools – from proper medications to coping skills – that reinforce your efforts. You deserve help; you don’t need to “tough it out” alone.
Example Scenario
Imagine Jane, who has chronic back pain. Initially, an injury caused her pain, and she stopped her daily walks and weekly meetups with friends. Over weeks, Jane became mostly homebound. Her muscles weakened and her mood sank – she often thought “My life is over; I can’t do anything.” When friends invited her out, she declined, afraid of hurting more or being seen as complainer. This led to loneliness and more focus on the pain. Recognizing the chronic pain cycle, Jane decided to try small changes. She started walking for 5 minutes in the morning (with her doctor’s okay) and doing a short breathing exercise at night. She also told a close friend that she misses them and arranged a quiet coffee catch-up. These small steps weren’t easy – her pain didn’t vanish overnight – but Jane noticed she felt a bit looser and lighter in mood after each walk, and the friendly chat lifted her spirits. Encouraged, Jane gradually increased her walks to 10 minutes and began attending a gentle yoga class online. Over time, these little changes added up: she felt a bit stronger, less depressed, and more engaged with life. The pain is still there, but it no longer dominates every aspect of her day. Jane essentially put a “spoke in the wheel” of the pain cycle, slowing it down and finding moments of relief and joy again.
Resources
Article: “Managing Chronic Pain with Cognitive Behavioral Therapy: A Comprehensive Guide“ by Western Reserve Hospital. An informative article detailing how cognitive behavioral therapy (CBT) can be an effective approach for managing chronic pain, emphasizing the importance of addressing both the physical and psychological aspects of pain.
Online Guide: “Chronic Pain Self-Help Guide“ by NHS Inform. A free online guide offering practical tips, exercises, and audio tracks for pain management, grounded in Cognitive Behavioral Therapy (CBT) and mindfulness techniques.
Book: “The Pain Management Workbook: Powerful CBT and Mindfulness Skills to Take Control of Pain and Reclaim Your Life” by Dr. Rachel Zoffness (2020). A friendly workbook combining CBT, mindfulness, and pain science to help individuals understand and manage chronic pain in daily life.
Podcast: “Curable“. A science-based podcast providing education and guided exercises for retraining the brain’s response to chronic pain, including meditation and writing exercises.
Video: “The Mystery of Chronic Pain“ by Dr. Elliot Krane (TED Talk, 2012). A TED Talk explaining how pain works in the nervous system, how chronic pain is different, and offering hope for change.
Website: “Breathworks“. Meditation programs specifically designed for chronic pain and illness, with guided practices like the “Body Scan for Pain” that teach mindfulness and compassion toward pain.